Dermatitis herpetiformis diagnosis and management begins with recognizing that this chronic, blistering skin condition is actually the skin-based form of celiac disease. Many people mistake the intense itching and red bumps for eczema or insect bites. However, this condition occurs because your immune system reacts to gluten by depositing antibodies in your skin. If you have these symptoms, you must address the root cause in your gut to clear your skin.
This condition is often called the “gluten rash.” It causes clusters of small, fluid-filled blisters that sting and burn. Because it is an autoimmune disorder, you cannot simply treat it with over-the-counter creams. Successful dermatitis herpetiformis diagnosis and management requires a combination of medical testing and strict lifestyle changes.
1. Recognizing the Physical Symptoms
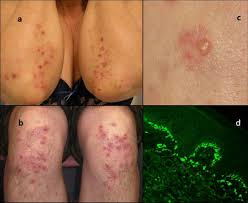
The first step in dermatitis herpetiformis diagnosis and management is identifying the classic physical signs. The rash is almost always symmetrical, appearing on both sides of the body simultaneously. You will likely find it on your elbows, knees, buttocks, or scalp.
Unlike other rashes, this one starts with an intense “burning” or “stinging” sensation. Small, red bumps then appear, quickly turning into tiny blisters. Because the itch is so severe, most people scratch the blisters until they scab over. This often makes it harder for doctors to see the original blister, which is why early reporting is so important.
2. The Gold Standard for Diagnosis
You cannot achieve proper dermatitis herpetiformis diagnosis and management without a specific skin biopsy. Doctors perform a “punch biopsy” on the healthy skin immediately adjacent to a lesion. They look for IgA antibody deposits that form a granular pattern under the microscope.
Many patients assume a blood test for celiac disease is enough. While blood tests are helpful, about 10% of people with this skin condition will have a negative blood test. Therefore, the skin biopsy remains the most reliable way to confirm you have the condition.
3. Medical Interventions and Dapsone
In the early stages of dermatitis herpetiformis diagnosis and management, doctors often prescribe a medication called Dapsone. This drug is highly effective at stopping the itch and clearing the blisters. Most patients feel relief within 24 to 48 hours of taking the first dose.
However, Dapsone does not cure the underlying gluten intolerance. It only treats the skin symptoms. It also requires careful monitoring because it can cause side effects like anemia. Doctors typically use Dapsone as a temporary measure while the patient transitions to a gluten-free diet, which is the only permanent solution.
4. The Lifelong Gluten-Free Diet
The cornerstone of dermatitis herpetiformis diagnosis and management is a strict, lifelong gluten-free diet. You must remove all traces of wheat, barley, and rye from your meals. Even a tiny amount of cross-contamination can trigger a new flare-up on your skin.
When you stop eating gluten, the IgA deposits in your skin slowly begin to disappear. This process takes time—sometimes months or even years. However, sticking to the diet allows you eventually to stop taking medications like Dapsone. It also protects your small intestine from the silent damage that celiac disease causes.
5. Identifying Hidden Triggers in Your Environment
Effective dermatitis herpetiformis diagnosis and management often involves looking beyond your dinner plate. Gluten can hide in places you might not expect. Check your medications, vitamins, and even your lip balms or toothpastes.
While gluten isn’t usually absorbed through the skin, it is very easy to accidentally ingest products used on your face or hands. For someone with this condition, even minute amounts matter. Switching to certified gluten-free personal care products provides an extra layer of safety for your immune system.
6. Monitoring for Associated Conditions
Part of long-term dermatitis herpetiformis diagnosis and management is watching for other autoimmune issues. Since your immune system is already prone to overreacting, you have a higher risk of developing thyroid disease or Type 1 diabetes.
Regular check-ups with your doctor are essential. They will monitor your bone density, as malabsorption from the gut can lead to osteoporosis. They will also check your iron and B12 levels to ensure your body is healing and absorbing nutrients correctly.
Comparison of DH vs. Other Skin Conditions
| Feature | Dermatitis Herpetiformis | Eczema | Shingles |
| Primary Cause | Gluten/Autoimmune | Allergies/Irritants | Viral (Varicella) |
| Symmetry | Always Symmetrical | Random | Follows Nerve Path |
| Itch Level | Extremely Intense | Moderate to High | Painful/Burning |
| Treatment | Gluten-Free Diet | Steroid Creams | Antivirals |
Healing the Gut to Clear the Skin
When you commit to dermatitis herpetiformis diagnosis and management, you are healing your entire body. The skin is simply the messenger. By repairing your gut through proper nutrition, you reduce systemic inflammation. This leads to clearer skin, higher energy levels, and better overall health.
Focus on whole foods such as:
- Fresh fruits and vegetables
- Lean meats and fish
- Beans and legumes
- Gluten-free grains like quinoa and rice
Avoid processed foods that may have “hidden” gluten in the thickeners or flavorings. Learning to read labels effectively is a skill that will serve you well for the rest of your life.
Conclusion
Successfully navigating dermatitis herpetiformis diagnosis and management requires patience and persistence. While the initial symptoms are incredibly frustrating, the path to healing is clear. By combining medical expertise with a dedicated gluten-free lifestyle, you can reclaim your skin health and protect your internal organs from damage.
For more information on managing autoimmune conditions and living a heart-healthy, gluten-free life, visit cardiachq.com. We provide the resources you need to stay informed and healthy every day.
Have you been struggling with a mystery rash that only goes away when you change your diet? Or are you currently looking for a doctor who understands the link between skin and gluten? Share your story in the comments below! We love hearing from our community and answering your questions.
Next Step for You:
Would you like me to generate a checklist you can take to your dermatologist to help start the process of a formal diagnosis?